Atopic dermatitis (AD) is a chronic, inflammatory cutaneous disease characterized by pruritus and generalized eczematous eruptions with frequent exacerbations and remissions. AD is associated with other atopic conditions such as food allergies, asthma, allergic rhinoconjunctivitis, eosinophilic esophagitis, and eosinophilic gastroenteritis. AD is most often the first step in the evolution of atopic diathesis. Early treatment of AD is strongly recommended with the hope that more severe associations may be prevented later in life.
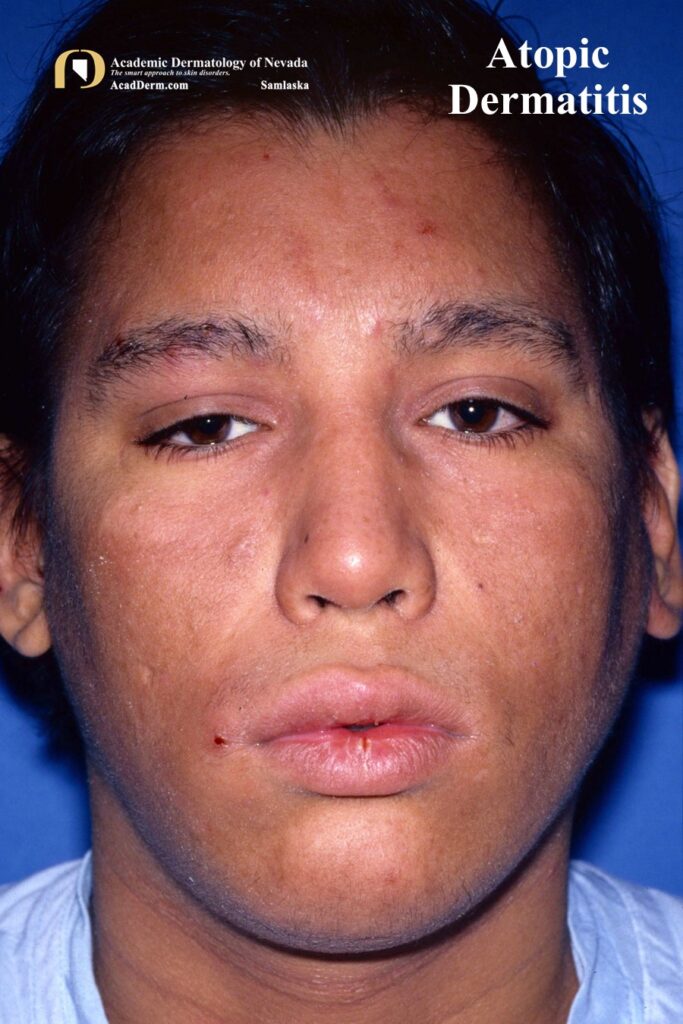

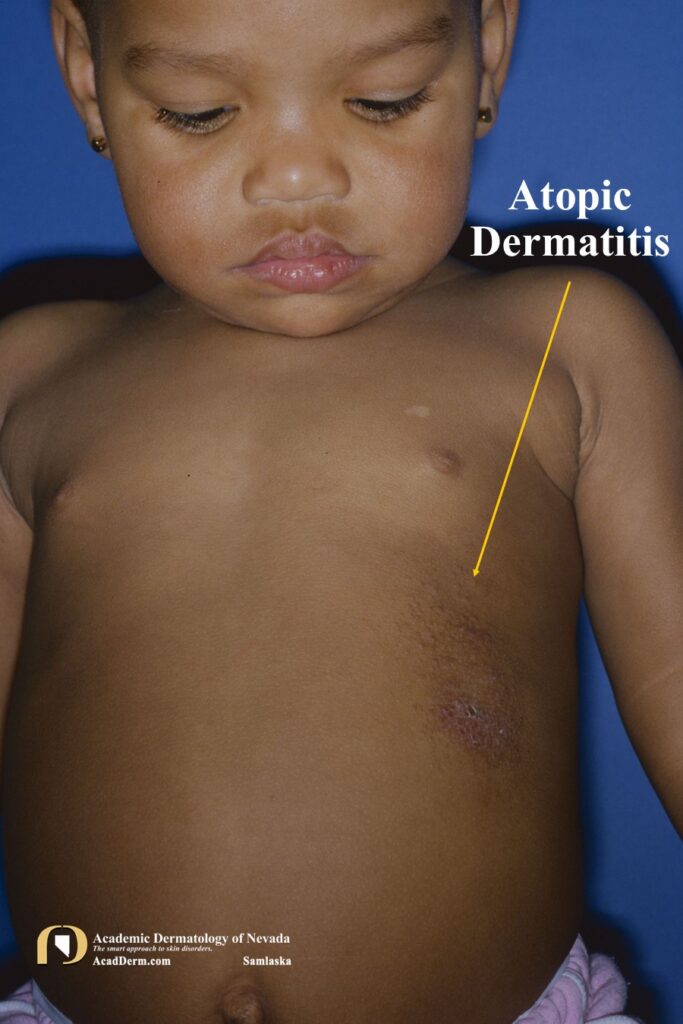
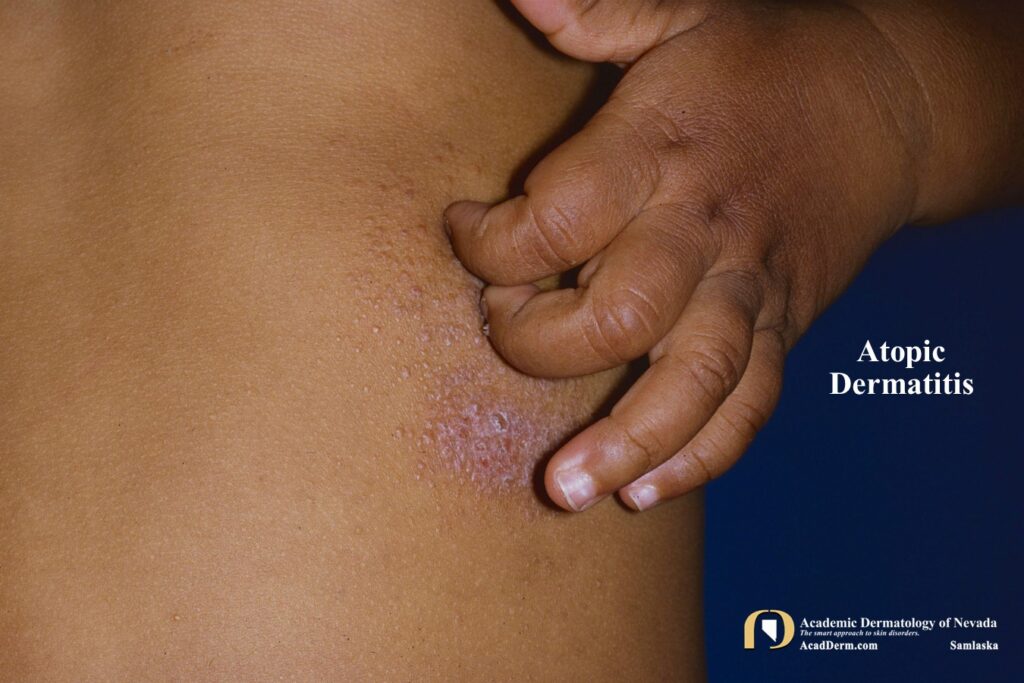
The prevalence of AD, asthma and allergic rhinoconjunctivitis has increased dramatically in the last half of the 20th century and is a major health problem in many nations. Girls are slightly more likely to develop AD with worldwide prevalence rates around 20-30% in the highest income nations and around 10% in other countries. About 50% of cases of AD appear in the first year of life, the vast majority within the first 5 years. In adults AD develops usually before the age of 30 years. Elevated IgE levels are not diagnostic of adult AD. Adult AD should be considered only when the dermatitis has a characteristic distribution and when other significant diagnosis have been excluded, such as allergic contact dermatitis, photodermatitis and cutaneous T-cell lymphoma.
Criteria for Atopic Dermatitis
MAJOR CRITERIA:
Must have three of the following:
1. Pruritus
2. Typical morphology and distribution
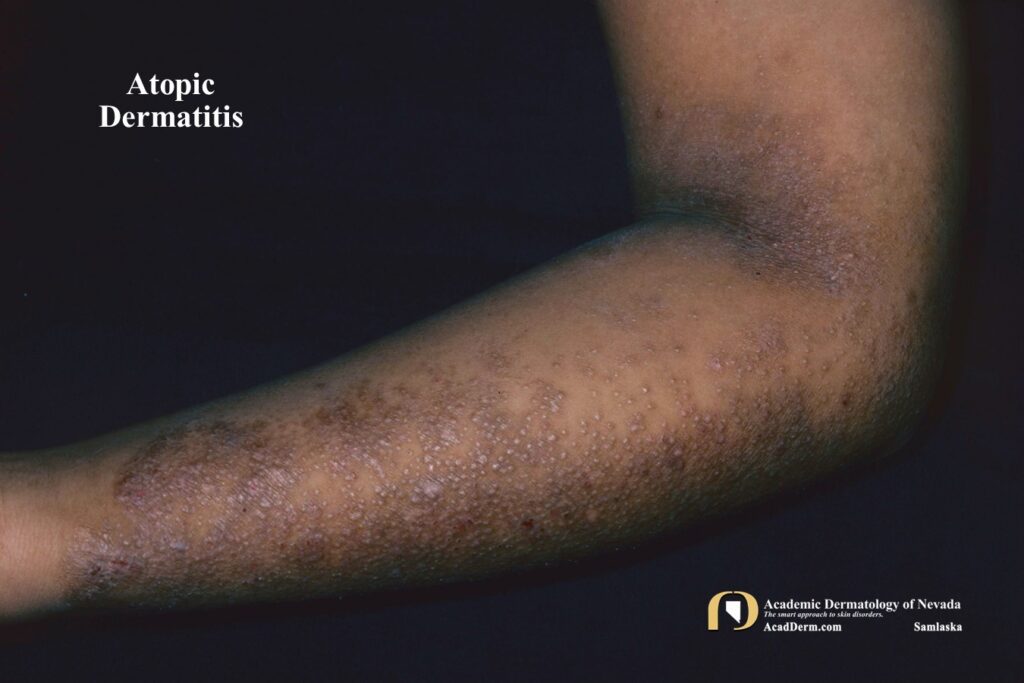
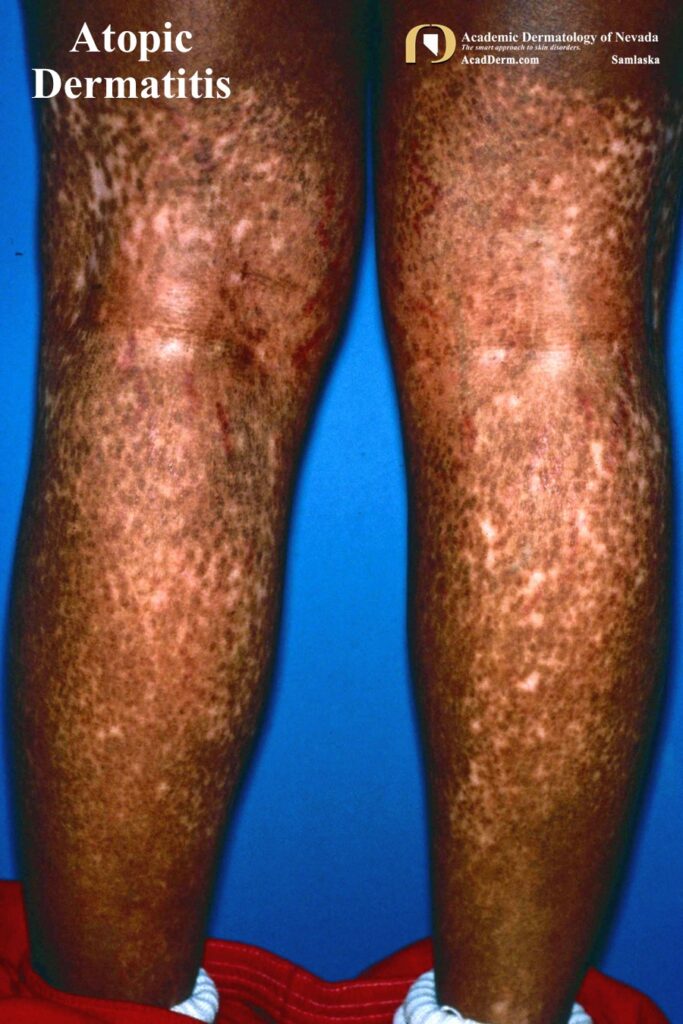
— Flexural lichenification in adults
— Facial and/or extensor involvement in infancy
3. Chronic or chronically relapsing dermatitis
4. Personal or family history of atopic disease (e.g., asthma, allergic rhinitis, atopic dermatitis
MINOR CRITERIA
1. Xerosis
2. Ichthyosis/hyperlinear palms/keratotsis pilaris
3. IgE reactivity (immediate skin test reactivity RAST test positive)
4. Elevated serum IgE
5. Early age of onset
6. Tendency for cutaneous infections (especially Staphylococcus aureus and HSV)
7. Tendency to nonspecific hand/foot dermatitis
8. Nipple eczema
9. Cheilitis
10. Recurrent conjunctivitis
11. Dennie-Morgan infraorbital fold
12. Keratoconus
13. Anterior subcapsular cataracts
14. Orbital darkening
15. Facial pallor/facial erythema
16. Pityriasis alba
17. Itch when sweating
18. Intolerance to wool and lipid solvents
19. Perifollicular accentuation
20. Food hypersensitivity
21. Course influenced by environmental and/or emotional factors
22. White dermatographism or delayed blanch to cholinergic agents.
ETIOLOGY: The etiology of AD is vast and beyond the scope of this post. The most important and frequently found association is that of a familial predisposition. For more information, please refer to the references below.
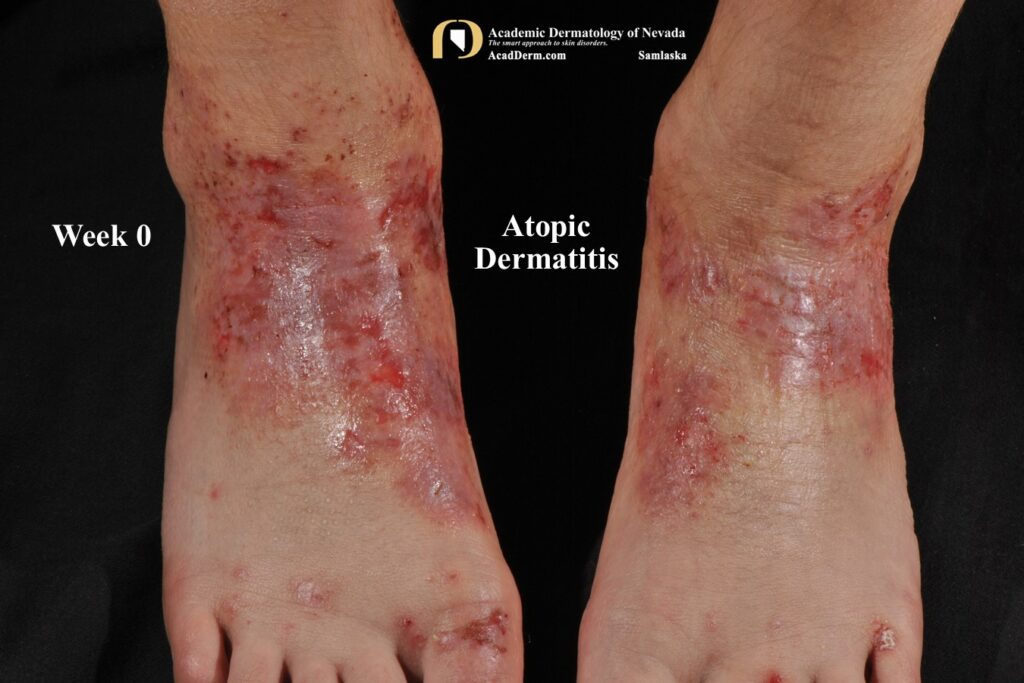
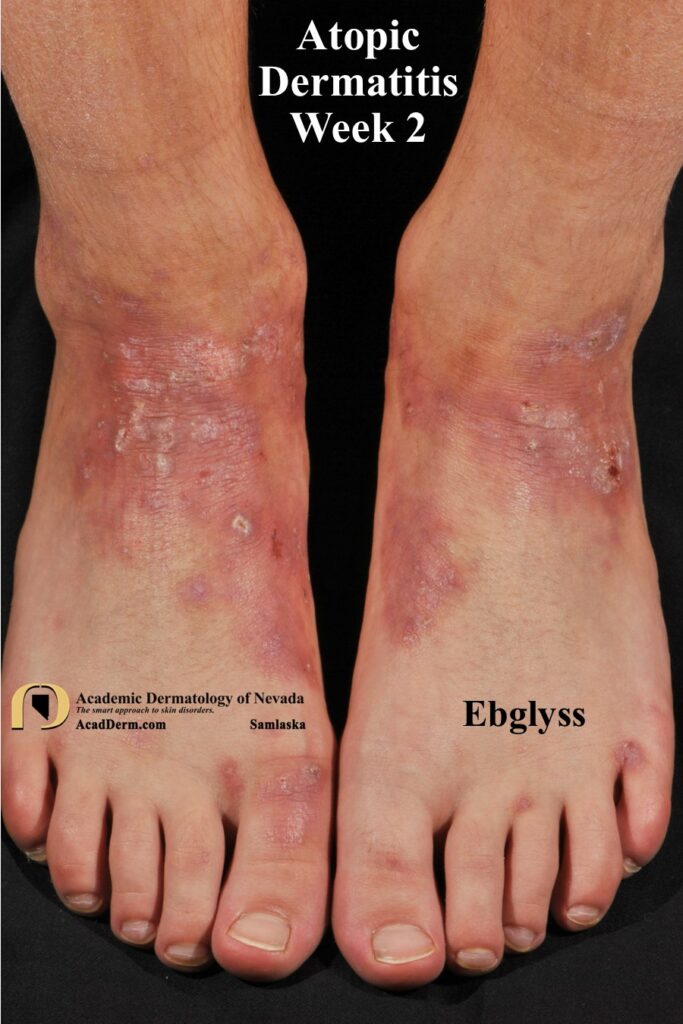
TREATMENT: The treatments required for the effective management of AD are vast and include many measures, such as control of environmental factors, soap and water precautions, multiple daily applications of bland moisturizers, etc. Again, reviewing all of the various treatment options is beyond the scope of this post and you should make an appointment with your dermatologist to instigate proper management. We are entering the golden age of treatment with the recent addition of JAK inhibitors for management of AD. AD can be a very severe disease with long-term complications. For more information on AD please go to HERE, HERE, and HERE.
